What's New at Veribrance
Discover tools and tips for running sleep centers with maximum efficiency. Explore Veribrance's expert insights, podcast interviews with industry leaders, and monthly newsletter for sleep operation managers.

We understand the financial complexities of running the operations of a sleep center. Built by sleep center RCM experts, Veribrance's (formerly Aarogram's) AI Agent automates benefits verification, provides accurate pre-visit estimates and improves upfront payment collection.
In-lab Sleep Study: Polysomnography (PSG)
Home Sleep Test (HST)
CPAP / Durable Medical Equipment (DME)
Office / Telehealth Consultation
Remote Patient Monitoring (RPM)
And More
Aarogram's AI platform is designed to address the inherent uncertainties in insurance estimates for neurology centers. Developed by RCM experts, it automates benefits verification, provides accurate pre-visit estimates and improves upfront payment collection.
EEG Testing
Ambulatory Testing
Epilepsy Testing
MRI
Injectables
And More
Aarogram's AI platform is designed to mitigate the insurance and patient payment uncertainty faced by physical therapy centers. Developed by RCM experts, it automates benefits verification, provides accurate pre-visit estimates and improves upfront payment collection.
Therapeutic Exercises
Therapeutic Procedures
Therapeutic Activities
Electrical Stimulation Therapies
Physical Therapy Evalution
And More
Aarogram's AI platform is designed specifically for mental health practices, addressing the challenges of insurance estimate uncertainty. Developed by RCM experts, it automates benefits verification, provides accurate pre-visit estimates and improves upfront payment collection.
Psychotherapy
Office Visit
Psychiatric Diagnostic Evaluation
Psychiatric Treatment
Psychiatric Services
And More
Aarogram's AI platform is designed to eliminate the uncertainty associated with insurance estimates at primary care practices. Developed by RCM experts, it automates benefits verification, provides accurate pre-visit estimates and improves overall upfront payment collection.
X-Ray Exam
Chest MRI
Patient Evaluation Complex
Annual Checkups
And More
Aarogram SmartVerify AI offers benefit verification automations and pre-service estimates designed specifically to enhance patient trust for digital health and tele-health services. We integrate seamlessly with existing workflows through API connections, enabling digital health providers to offer accurate benefit verification and clear price estimates.
Remote Patient Therapy (RTM)
Tele-health Consultation
Tele-health Sleep Therapy
Tele-health Physical Therapy
And More
Aarogram's AI platform is designed to eliminate the uncertainty associated with insurance estimates at Pulmonology clinics. Developed by RCM experts, it automates benefits verification, provides accurate patient estimates and improves overall instant payment collections.
Basic Spirometry Test
Chest CT Scan
Oxygen Saturation
Bronchodilation Responsiveness
Pulmonary Stress Testing
And More
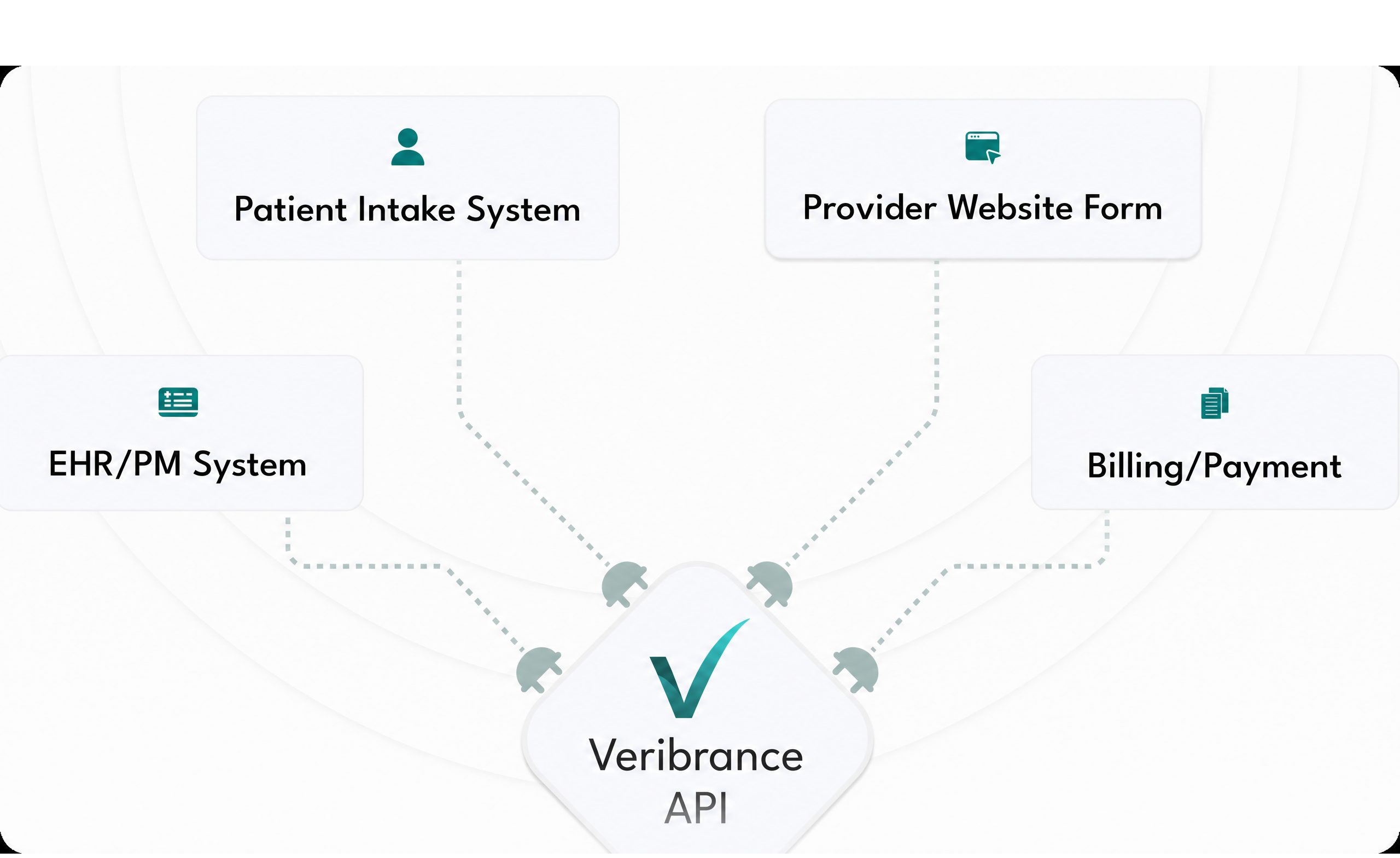
Are you a developer looking to integrate Veribrance's SmartVerify AI within your health tech platform?
Learn More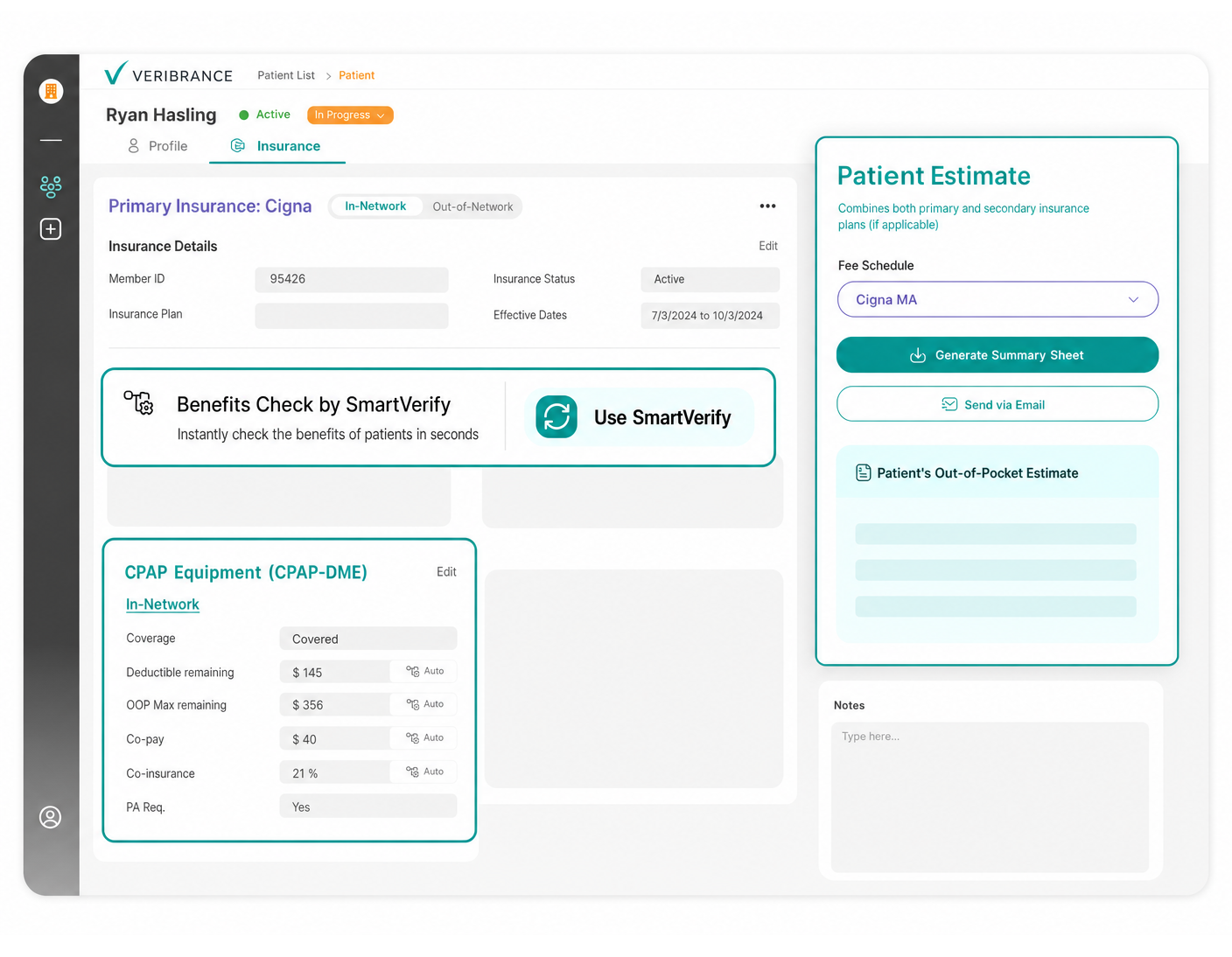
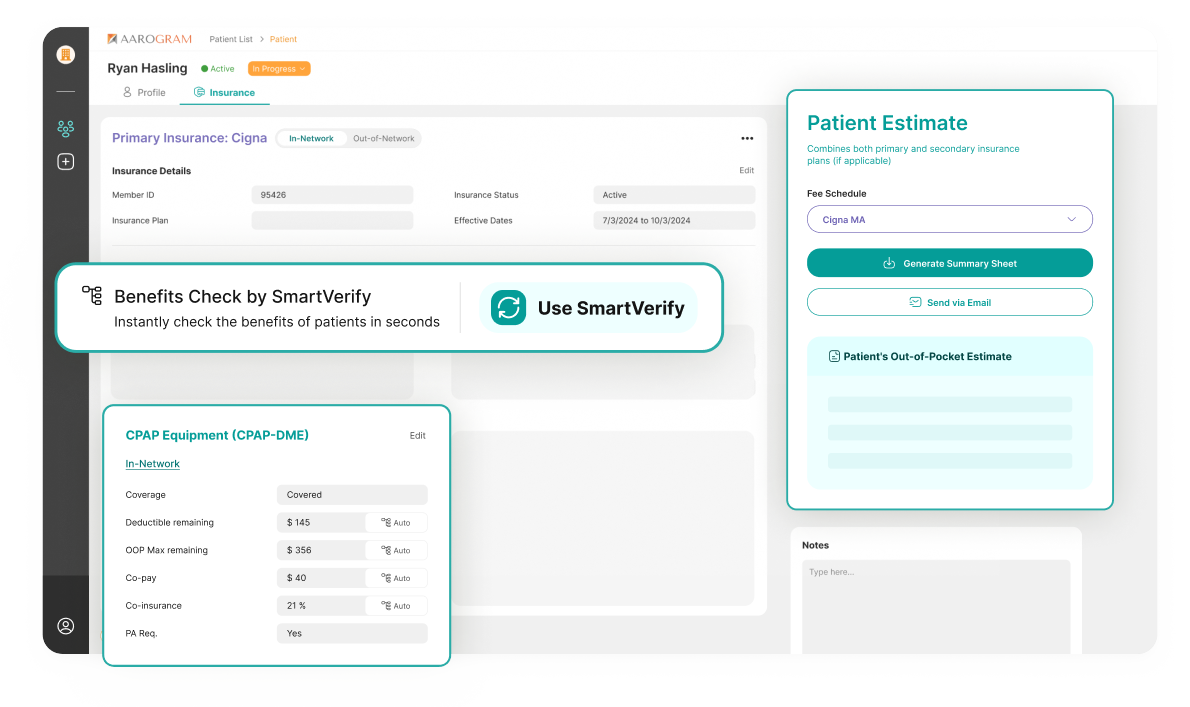















Discover tools and tips for running sleep centers with maximum efficiency. Explore Veribrance's expert insights, podcast interviews with industry leaders, and monthly newsletter for sleep operation managers.
Healthcare practices across the country trust Veribrance (formerly Aarogram) to simplify financial clearance for their patients and optimize their collection. Use it with your current EHR, your staff or your billing company - your choice. Curious to know how we do it?
AI Agent for Benefits Verification (>95% Accuracy)
Real-time Patient & Insurance Estimates
Cost Estimator for Provider Website