Get Started

Solutions
By Specialties
Sleep
Neurology
Physical Therapy
Mental Health
Dental
Digital Health
Urgent Care
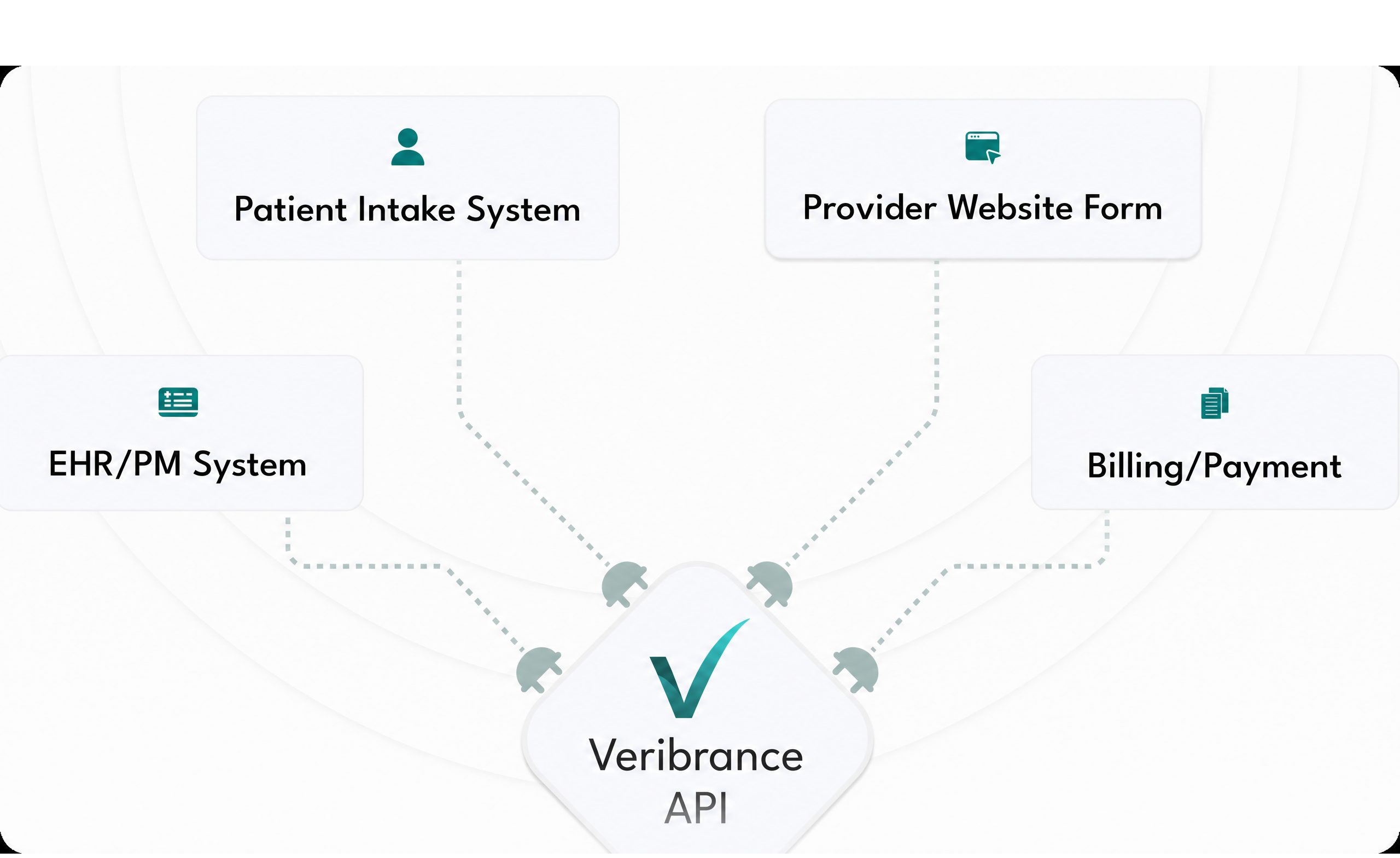
For Developers & Health Tech Platforms
Resources
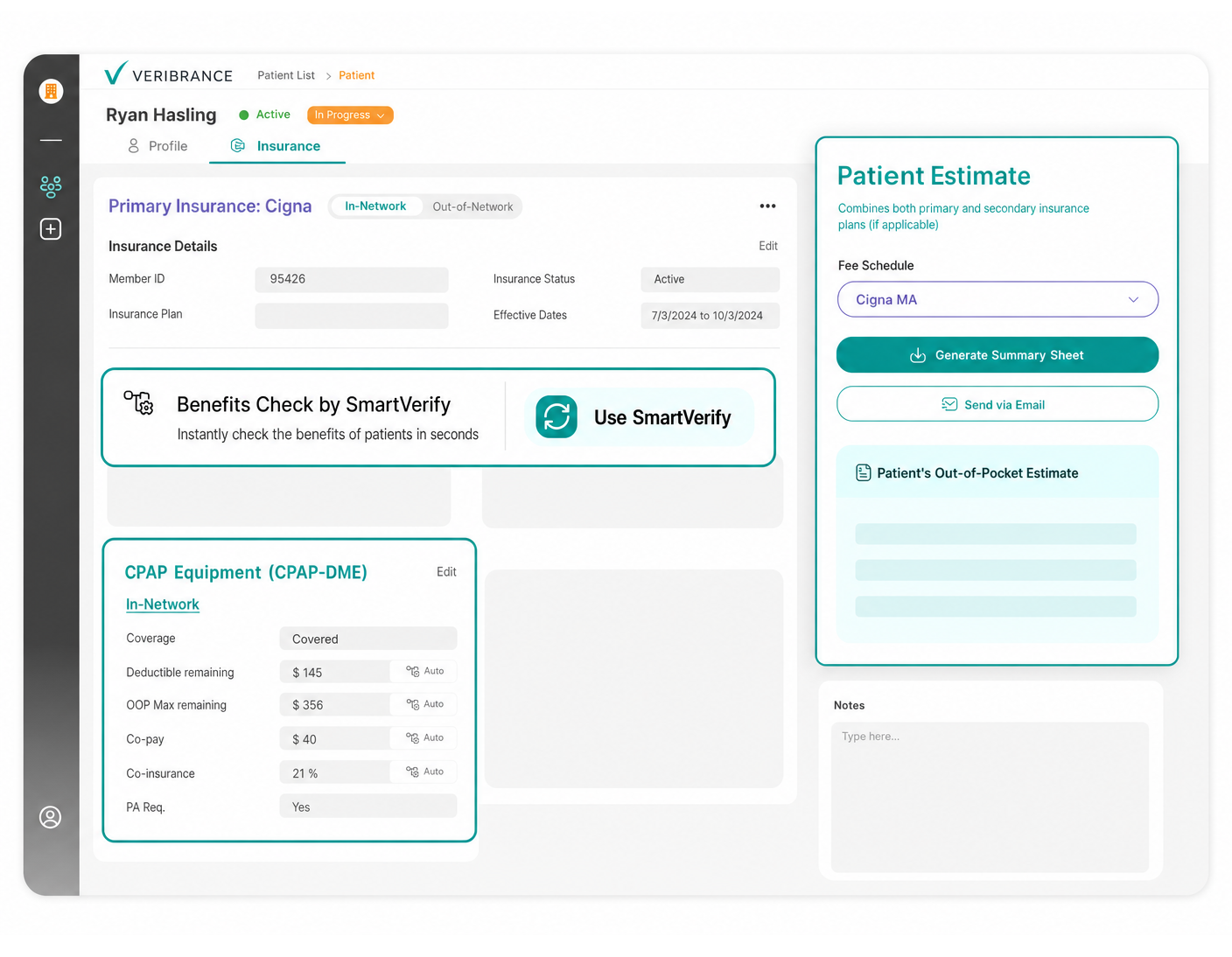
Patient Estimate Calculator
Staffing Cost RoI Calculator
Insurance Verification Contact Directory for Providers
Aarogram Blog
The Efficient Care Podcast














.svg)
.png)
.png)

.png)